
The results were analyzed with r Pearson. They were divided into 3 groups depending on the serum potassium concentration: 1) 5 to 5.9 mEq/L, 2) 6 to 6.9 mEq/L and 3) above 7 mEq/L, the PR and QT intervals, QRS complex, heart rate, the T wave abnormalities and rhythm were measured on the electrocardiogram. Material and methods: 52 patients with chronic renal failure and hyperkalemia were studied. the serum potassium levels in patients with chronic renal failure. Objective: To determine the correlation between the electrocardiographic alterations and. The electrocardiographic alterations are well known and they are related to the increasing in serum potassium levels, the nephropaty patients have more tolerance. Renal dysfunction by enhancing hyperglycemia and reducing potassium excretion also contributes to hyperkalemia.īackground: Hyperkalemia is a frequent alteration in hospitalized patients that increases the morbidity and mortality due to its cardiotoxicity. Since exogenous ketoacidemia and hyperglycemia in the otherwise normal experimental animal do not increase p, it is postulated that insulin deficit itself may be the major initiating cause of the hyperkalemia that develops in DKA. These results indicate that the endogenous ketoacidemia and hyperglycemia observed in DKA, which result primarily from insulin deficit, are the main determinants of increased p. The equation that best describes p on admission for DKA was: p = 25.4 - 3.02 pH + 0.001 G + 0.028 AG, (r = 0.515). Only plasma pH, glucose and AG emerged as having a definite independent effect on p, with no independent role found for bicarbonate, BUN and osmolality. Since the parameters under study are themselves interrelated, having statistically significant correlations with each other, their possible independent role on p was evaluated by multiple regression analysis. Significant (p less than 0.01) correlations of p with each of these parameters were found that could individually account for 8 to 15 percent of the observed variance in the plasma potassium levels however, the effects of some or all of these parameters on the p could be independent and therefore physiologically additive.

This study of 142 admissions for DKA examines the possible role of alterations in plasma pH, bicarbonate, glucose (G), osmolality, blood urea nitrogen (BUN) and plasma anion gap (AG) on the levels of p on admission. However, several metabolic derangements other than volume depletion and acidosis, which are known to alter potassium metabolism, also develop in DKA. It has been suggested, instead, that the elevated serum of DKA might be the result of the compromised renal function, secondary to volume depletion, that usually accompanies DKA. The classic proposal of intracellular K+ for extracellular H+ exchange as responsible for the hyperkalemia of diabetic ketoacidosis (DKA) has been questioned because experimentally induced organic anion acidosis fails to produce hyperkalemia. Therefore, clinicians should be careful that ECG may look normal in the presence of severe hyperkalemia. Our case confirms that diagnostic ECG changes do not always accompany severe hyperkalemia. Our case is particularly interesting because it demonstrates an Addison patient that has an extremely high level of K + (>10 mmol/L) without any accompanying ECG changes. Results of repeated ECGs have revealed a normal sinus rhythm. The patient's serum K + level was found to be at the highest level that can be detected in our laboratory (>10.0 mmol/L, normal 3.5-4.5 mmol/L) and repeated serum K + confirmed the previous result. A 40-year-old woman with AD was admitted to emergency service with generalized pain. Severe hyperkalemia secondary to Addison Disease (AD) is rare.
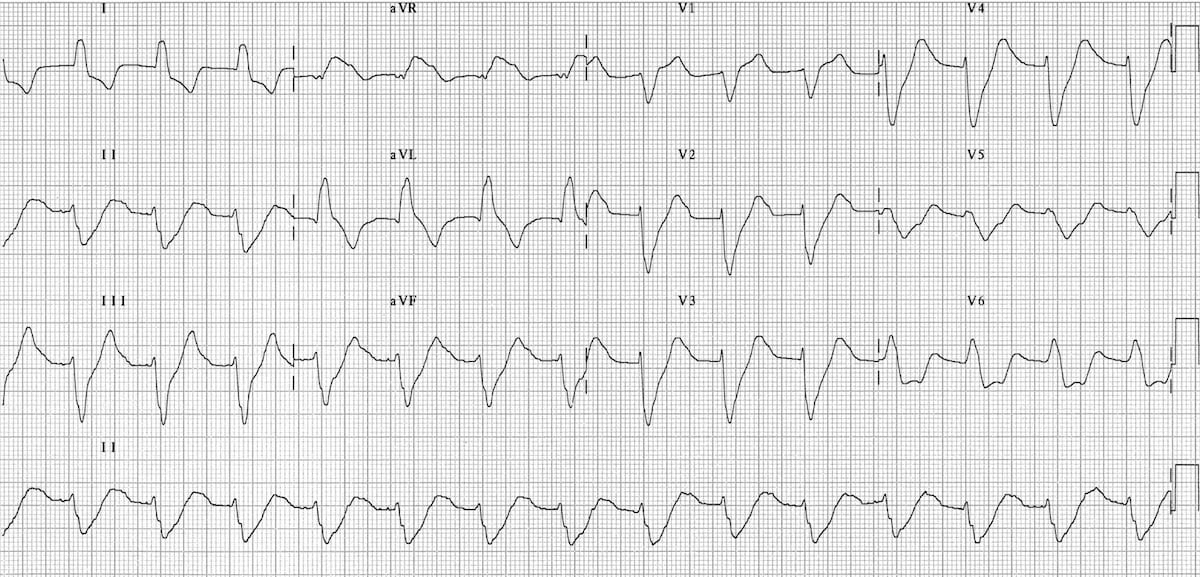
But in some patients ECG changes do not accompany serum K + abnormalities. Alterations in serum potassium (K +) levels can have dramatic effects on cardiac cell conduction and may lead to electrocardiographic (ECG) changes. Hyperkalemia is one of the most common acute life-threatening metabolic emergencies.
